India’s Transformation into a Global Health Powerhouse
India’s Transformation into a Global Health Powerhouse
Key Takeaways
Introduction
From conquering longstanding public health challenges to becoming a leading force in affordable medicines and global healthcare delivery, India’s rise as a global health powerhouse stands as a testament to visionary leadership, resilient institutions, and the unwavering commitment of the Government of India to building a healthier, stronger, and more prosperous nation. The Government runs flagship schemes that provide public health insurance, free healthcare and services across all levels and subsidised medicines, along with a widespread and accessible health infrastructure. The guiding principle is to provide universal health coverage – ensuring that everyone, including the most socio-economically disadvantaged populations, gets access to affordable and quality healthcare so that India can progress towards its goal of being a healthy, productive and prosperous society – a Viksit or developed Bharat – by 2047.
India’s medical education system, comprising private colleges along with publicly funded institutions, has seen expansion and growth over the years. India’s pharmaceutical sector, the world’s third largest by volume, enables a ready supply of affordable medicines not just to Indian citizens but also to the world – as evidenced by India’s prowess in manufacturing and supplying COVID-19 vaccines. India’s biopharmaceutical sector is growing in leaps and bounds, supported by government investment and private industry’s innovative spirit. India has been witnessing a rise in medical tourists, from over 112,000 in 2009 to over 600,000 in 2024. To enhance India’s medical tourism sector, the Government of India in its Union Budget 2026-27 announced the establishment of five integrated medical hubs across India featuring diagnostic infrastructure and rehabilitation services in partnership with the private sector. India is now poised to contribute more significantly to global public health – a remarkable achievement for a country that was battling endemic diseases not even a century ago.
Providing Universal Health Coverage: Ayushman Bharat
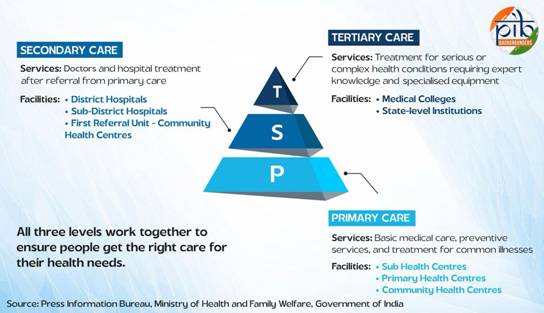
The Government of India’s flagship scheme – Ayushman Bharat (Long Live India) – is key to its aim in providing universal health coverage to all, particularly the socio-economically backward and vulnerable sections of the Indian society. This umbrella scheme has various components that work together to ensure that people get access to quality healthcare at all levels – primary, secondary and tertiary levels.
It’s four major components include
Pradhan Mantri Jan Arogya Yojana (Prime Minister’s People Health Programme)
The Government of India launched the Ayushman Bharat – Pradhan Mantri Jan Aarogya Yojana (AB-PMJAY) on September 23, 2018, to achieve universal health care. It is the world’s largest public healthcare scheme with hundreds of millions of vulnerable Indian families enrolled in it.
AB-PMJAY provides healthcare coverage up to Rs. 5 lakhs per year (~$5,000 USD) for secondary and tertiary care services and hospitalisation to enrolled socio-economically deprived families and to all senior citizens above 70 years, saving them from catastrophic medical bills. The scheme provides cashless treatment across empanelled government-funded and private hospitals. The scheme is aimed at the bottom 40% of the Indian population, covering 120 million people, with over 434 million Ayushman cards already made.

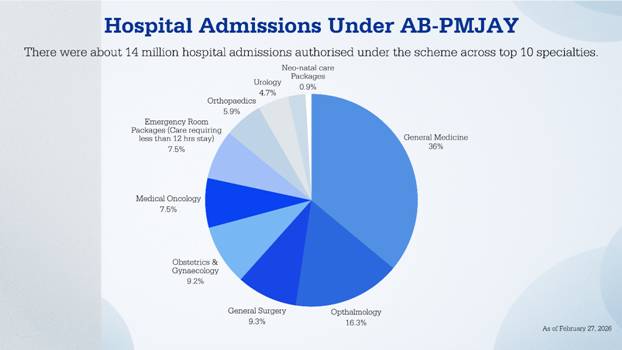
The scheme has helped reduce the healthcare expenditure of families by increasing government spending on health insurance. The savings for families was over Rs. 1.25 lakh crore (2024-2025) (~$13.77 billion USD).
The allocation for the Pradhan Mantri Jan Arogya Yojana has been raised to Rs. 9,500 crore (~$1.05 billion USD) in Budget Estimates 2026–27, up by Rs. 500 crore (~$55 million USD) or 5.56% over the Revised Estimates of Financial Year 2025–26. This increase aims to expand beneficiary coverage, improve service quality, and strengthen hospital networks.
While AB-PMJAY supports secondary and tertiary healthcare, the Ayushman Bharat scheme runs various other programmes to ensure quality primary healthcare and a robust healthcare infrastructure which is accessible to all.
Ayushman Arogya Mandirs
A strong primary care infrastructure ensures health equity and access. Ayushman Arogya Mandirs are primary health care centres under the Ayushman Bharat scheme that provide a wide range of general health services for people close to their homes.
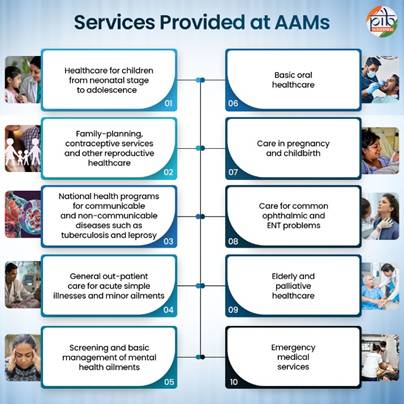
There are 1,84,235 AAMs across the country (as on February 27, 2026), including in the urban, rural and tribal-dominated areas. There are 30,817 AAMs in 178 tribal districts across 26 states and 24,327 AAMs in 112 aspirational districts across 27 states (as on December 31, 2025).
To ensure healthcare access, teleconsultations are also provided at AAMs – 426.6 million consultations have been conducted last year (as on December 31, 2025).
AAMs are where the community can access preventive and promotive healthcare. Over 58 million wellness sessions with yoga were also held at AAMs for the holistic development of people. The ministry screens millions of people for various non-communicable diseases under the National Programme for Prevention and Control of Non-Communicable Diseases. As on October 31, 2025, these are the number of screenings for various ailments:
Pradhan Mantri-Ayushman Bharat Health Infrastructure Mission
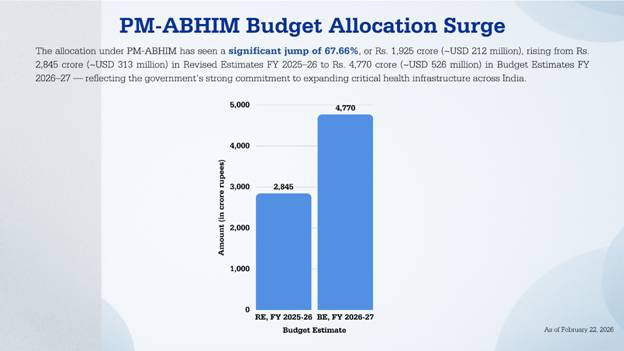
Recognising the vital role of AAMs in mitigating and controlling the impact of pandemics or other disease outbreaks, the Government of India launched the Pradhan Mantri–Ayushman Bharat Health Infrastructure Mission (PM-ABHIM) in 2021. PM-ABHIM looks at infrastructure in health, research and surveillance.
PM-ABHIM aims at strengthening the health infrastructure from the grassroots to the district level through establishment and upgradation of the following in every district:
PM-ABHIM also prioritises pandemic and disaster preparedness by expanding an IT-enabled, real-time disease surveillance network that integrates laboratories at block, district, regional, and national levels to detect, investigate, and prevent outbreaks effectively.
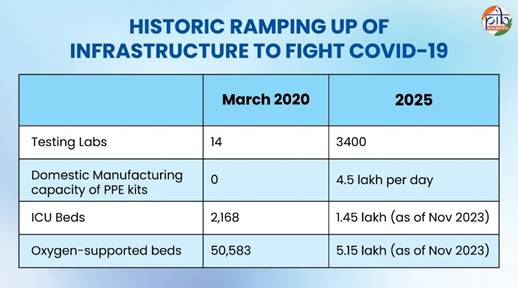
The Government of India approved Rs. 32,928.82 crore (~$3.63 billion USD) for a 5-year period from the fiscal years 2021-22 to 2025-26. This fund is for the construction, upgradation and establishment of:
Digital Initiatives – Ayushman Bharat Digital Mission and Technology Integrations
The Ayushman Bharat also supports the creation of a robust digital public infrastructure through the Ayushman Bharat Digital Mission (ABDM), one of the most ambitious digital health architectures in the world. Beneficiaries are assigned a unique health identification number, under the Ayushman Bharat Health Account (ABHA) system, enabling their medical records to be securely stored and accessed online through a “digital health locker”.
Over 863 million ABHAs have been created to date (as on February 27, 2026). Through an app, users can also connect with registered healthcare professionals. Verified healthcare  professionals can treat patients remotely through teleconsultations and review digital health records. This digital ecosystem enables the last-mile health coverage.
professionals can treat patients remotely through teleconsultations and review digital health records. This digital ecosystem enables the last-mile health coverage.
India runs one of the world’s largest digital mental health initiatives, operating 53 cells across all 36 states and union territories with 24×7 counselling services in 20 languages and having handled over 3.28 million. Launched on October 10, 2022, Tele MANAS has further expanded accessibility with support in 12 languages, providing comprehensive mental health support from general well-being to disorder management.
Revolutionising Healthcare Access: Drone-Based Delivery of Medical Services
 Pilot projects using drones are in process. In 2021, the Indian Council of Medical Research launched the ‘i-DRONE’ initiative to test drone-based delivery of vaccines and medical supplies to hard-to-reach areas in the mountainous states of Manipur and Nagaland. Following successful pilots across diverse terrains, the programme expanded nationwide with specialized applications: high-altitude medical deliveries in Himachal Pradesh (above 10,000 feet), TB sample transport in Telangana to reduce diagnostic time, pathological sample transfers in Karnataka for time-sensitive cases, and blood product transportation studies in Delhi NCR. These initiatives demonstrate how drones can strengthen last-mile healthcare connectivity, accelerate diagnostics, and provide critical medical logistics support in challenging geographies.
Pilot projects using drones are in process. In 2021, the Indian Council of Medical Research launched the ‘i-DRONE’ initiative to test drone-based delivery of vaccines and medical supplies to hard-to-reach areas in the mountainous states of Manipur and Nagaland. Following successful pilots across diverse terrains, the programme expanded nationwide with specialized applications: high-altitude medical deliveries in Himachal Pradesh (above 10,000 feet), TB sample transport in Telangana to reduce diagnostic time, pathological sample transfers in Karnataka for time-sensitive cases, and blood product transportation studies in Delhi NCR. These initiatives demonstrate how drones can strengthen last-mile healthcare connectivity, accelerate diagnostics, and provide critical medical logistics support in challenging geographies.
National Health Mission
Apart from the umbrella Ayushman Bharat scheme, the Government of India has been running the National Health Mission for decades, with its two components – the National Urban Health Mission and the National Rural Health Mission – for the prevention, mitigation and treatment of various kinds of diseases. The National Health Mission (NHM) has significantly contributed to improving India’s public health outcomes through its relentless efforts in expanding human resources, addressing critical health issues, and fostering an integrated response to health emergencies.
The NHM works to improve maternal, child, and adolescent health through programmes including immunisation, strengthens health systems by improving quality standards, and manages a range of communicable and non-communicable diseases (NCDs) control programmes.
Universal Immunisation Programme
The Universal Immunisation Program (UIP) is one of the largest public health programs targeting close of 26.7 million newborns and 29 million pregnant women annually free of cost.
Strategic interventions like advocacy, social mobilisation, inter-personal communication at the family level by community health workers and media engagement are some measures utilised to improve immunisation coverage. Community health workers called the Accredited Social Health Activists and Auxiliary Nurse Midwives conducted over 13 million immunisation sessions across the country. There are over 1.03 million ASHAs working under the NHM across the country (as of April 4, 2025).
The 11 vaccines given under the programme are:
HPV Vaccination Programme Launched
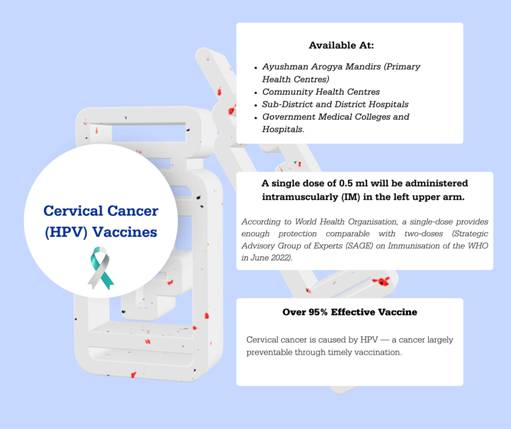
The Government of India launched a three-month nationwide HPV Vaccination Programme on February 28, 2026, for the prevention of cervical cancer among women. The Gardasil-4 vaccine, which is a single-dose, WHO pre-qualified vaccine used in immunisation programmes across the world, is now being given to adolescent girls aged 14 years, free of cost, at all government primary and community health centres, district and sub-district hospitals, and government medical colleges and hospitals across the country through central-state/UT government collaboration. Gardasil-4, a quadrivalent HPV vaccine protects against HPV types 16 and 18 (which cause cervical cancer), as well as types 6 and 11.
About 11.5 million girls are presently eligible for the vaccine. The 90-day vaccination drive is running daily to ensure maximum coverage and will thereafter be available on routine immunisation days. This nationwide HPV vaccination campaign is a pivotal step towards empowering India’s women and safeguarding the health of mothers and daughters across the country. With this landmark campaign, India has joined over 160 countries with HPV vaccination programmes.
Mission Indradhanush
Mission Indradhanush was launched on December 25, 2014 under the Universal Immunisation Programme (UIP) to immunise children and pregnant women who have either missed or dropped out of routine immunisation schedules, focusing on regions with low vaccination coverage.
As a result of the continued, sustained efforts and intensified implementation of vaccination drives and campaign across the country, the percentage of zero-dose children to the total population has declined from 0.11% in 2023 to 0.06% in 2024.Recent data on MI vaccination numbers.
Other NHM Programmes, Infrastructure and Impact
Other than the immunisation programme, the National Health Mission runs a wide network of programmes for all kinds of ailments and health conditions.

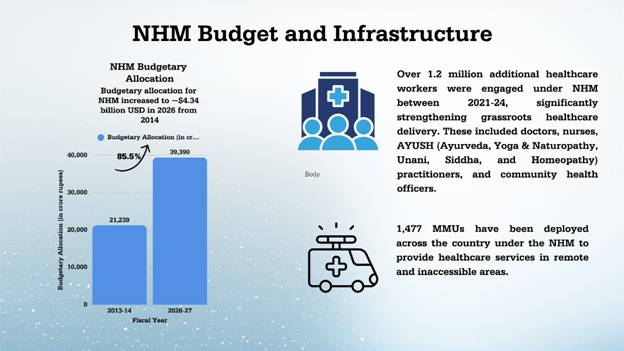
Budgetary Increase
Increase in NHM funding and capacity building has resulted in the improvement of India’s public health indicators over the past few decades.
Key Achievements of National Health Mission:
Integration of Artificial Intelligence in Healthcare
From 2022 to 2025, India has fundamentally restructured its public health delivery by integrating artificial intelligence (AI) into a unified strategy, that bridges specialist shortages and scales proactive care. In February 2026 during the AI Summit in New Delhi, the Ministry of Health and Family Welfare launched the Strategy for AI in Healthcare for India (SAHI), the first nation in the South-Eastern region to do so. The strategy encourages innovation and rapid increase in the application of AI in healthcare, while emphasising ethical use and conduct. The Government of India has already integrated AI into its ABDM infrastructure and other programmes.
Artificial intelligence is increasingly being operationalised across disease areas and health system functions in India. Some examples are:
Making Medicines Affordable
Apart from making healthcare more accessible and affordable, the Government of India makes available quality generic medicines at affordable prices through the Pradhan Mantri Bhartiya Janaushadhi Pariyojana (PMBJP). The medicines are available at the 17,990 Janaushadhi Kendras country wide. Over 2,000 medicines and 315 surgical products are available at the Kendras and are sold at 50-90% lower rates than the market price. These medicines provide treatment for a range of diseases and ailments, such as cardiovascular diseases, cancer, diabetes and others. The scheme has saved beneficiaries about Rs. 30,000 crores (~$3.31 billion USD) in the past decade.
To complement the PMBJP, the government launched the Affordable Medicines and Reliable Implants for Treatment (AMRIT) initiative, aimed specifically at supporting tertiary healthcare. AMRIT Pharmacies act as centralised supply points for branded, branded-generic, and generic drugs, as well as surgical items, consumables, and medical implants—especially those required for high-end treatments. There are 255 pharmacies in India, with a vision to expand this network to 500 outlets across the country (as of November 2025).
Pharmacy of the World
India’s strong pharmaceutical sector, the 3rd largest in the world by volume, has enabled it to become the largest supplier of generic medicines providing 20% of the world’s supply. The country exports to about 200 countries and territories. India is also a key player in affordable vaccines.
For the Global South, India’s pharmaceutical supplies – low cost and of good quality – provides essential health security. The country currently supplies over 70% of global anti-retroviral medicines, ensuring affordable access for nations in need.
The Central Drugs Standard Control Organisation (CDSCO), along with the National Regulatory Authority of India (NRA) and affiliated institutions, were found to meet the World Health Organisation’s published indicators for a functional vaccine regulatory system in October 2024.
During the COVID-19 pandemic, India developed indigenous vaccines including Covaxin and Covishield, demonstrating its unique capacity to integrate research and large-scale production.
India’s pharmaceutical sector has long been a global vaccine supplier, providing 55–60% of UNICEF’s vaccines and meeting a significant share of global demand for DPT, BCG, and measles vaccines, saving millions of lives across continents.
India is now using biotechnology to manufacture high-value biologics, biosimilars and innovative therapeutics. India’s bio-economy sector has seen a 13-fold increase over the past decade, from $10 billion USD in 2014 to over $165.7 billion USD in 2024 and is projected to reach $300 billion USD by 2030.
The Union Budget 2026–27 lunched of Biopharma SHAKTI, designed to strengthen India’s end-to-end ecosystem for biologics and biosimilars through investments in domestic manufacturing, workforce development, a nationwide network of over 1,000 accredited clinical trial sites, and enhanced regulatory capacity at the Central Drugs Standard Control Organisation (CDSCO). Three new National Institutes of Pharmaceutical Education and Research (NIPERs) will be established, and seven existing ones upgraded, to meet the growing demand for specialised human resources in biopharma. This initiative, along with existing National Biopharma Mission, aims to catalyse India’s global role in the next industrial revolution and establish India as a global biomanufacturing hub.
The National Biopharma Mission (NBM)—”Innovate in India (i3)”—has already catalysed transformative outcomes since its launch in 2017. Co-funded by the World Bank and implemented by the Biotechnology Industry Research Assistance Council (BIRAC), the Mission supports 101 projects involving over 150 organisations and has generated more than 1,000 jobs, including 304 scientists and researchers. Breakthroughs include India’s first indigenously developed MRI scanner at a fraction of the cost of imported machines, the country’s first biosimilar of Liraglutide for Type 2 diabetes priced at nearly one-third of the imported version, and the world’s first DNA-based COVID-19 vaccine, ZyCoV-D, developed by Zydus Cadila. These innovations are India’s contribution to making quality healthcare more affordable.
Health Education Expansion
Due to the growing medical sector and rising demand for services, the Government of India is systematically expanding medical education to keep pace. Over the past 11 years, the Government of India made gains in making quality medical education more accessible. There are now 23 publicly funded and leading All India Institute of Medical Sciences institutes, including the first-ever AIIMS in the northeastern area in Assam. There are 2,045 medical colleges, including 780 allopathy, 323 dental and 942 AYUSH institutions. Medical education seats for the MBBS (Bachelor of Medicine and Bachelor of Surgery) increased by 130% (from 51,348 to 118,190), and postgraduate seats grew by 138% (from 31,185 to 74,306).
Conclusion
India’s transformation from a nation battling endemic diseases to a global medical tourism hub and health technology leader demonstrates what strategic government intervention can achieve. The infrastructure built—from over 180,000 Ayushman Arogya Mandirs to the world’s largest digital health ecosystem with over 860 million health IDs—has not only improved health outcomes domestically but positioned India as a destination for quality, affordable healthcare worldwide. As the nation moves toward its 2047 vision of Viksit Bharat, the foundation is firmly in place: robust public health systems, cutting-edge digital architecture, and an unwavering commitment to ensuring that every citizen, regardless of geography or income, has access to quality healthcare—making India a model for health equity in the developing world.
References
- AB–Pradhan Mantri Jan Arogya Yojana (PM-JAY), the world’s largest publicly funded health assurance scheme.
- Ayushman Arogya Mandir for upgrading sub health centres and primary health centres.
- Pradhan Mantri Ayushman Bharat Health Infrastructure Mission (PM-ABHIM) – the largest pan-India scheme for strengthening healthcare infrastructure across the country.
- Ayushman Bharat Digital Mission (ABDM), which forms the backbone for a citizen centric interoperable digital health ecosystem.